Insulin is a vital hormone produced by the pancreas that plays a central role in regulating blood sugar levels in the body. Its primary function is to facilitate the uptake of glucose (sugar) from the bloodstream into cells to be used as energy or stored for later use. Insulin acts as a key that unlocks cells, allowing glucose to enter and fuel essential bodily functions.
When food is consumed, especially carbohydrates, the body breaks it down into glucose, which enters the bloodstream. In response, the pancreas secretes insulin into the bloodstream. Insulin then signals cells throughout the body, prompting them to absorb glucose, thus reducing the amount of glucose in the blood.
Insulin deficiency or the body’s inability to properly use insulin leads to diabetes, a condition characterized by elevated blood sugar levels. Type 1 diabetes results from the immune system attacking and destroying the cells in the pancreas that produce insulin. In contrast, type 2 diabetes occurs when the body becomes resistant to insulin or doesn’t produce enough to meet its needs.
Individuals with type 1 diabetes require insulin injections or use insulin pumps to manage their blood sugar levels because their bodies cannot produce this hormone. In type 2 diabetes, treatments may involve lifestyle modifications, oral medications, or, in some cases, insulin therapy to supplement the body’s insulin production.
Insulin formulations have evolved over the years, offering different types with varying onset times and durations of action. Rapid-acting insulin starts working within minutes and is taken just before or after meals to manage post-meal glucose spikes. Long-acting insulin provides a steady background level of insulin over an extended period, mimicking the body’s basal insulin production. These different types of insulin allow for customized treatment regimens tailored to an individual’s needs.
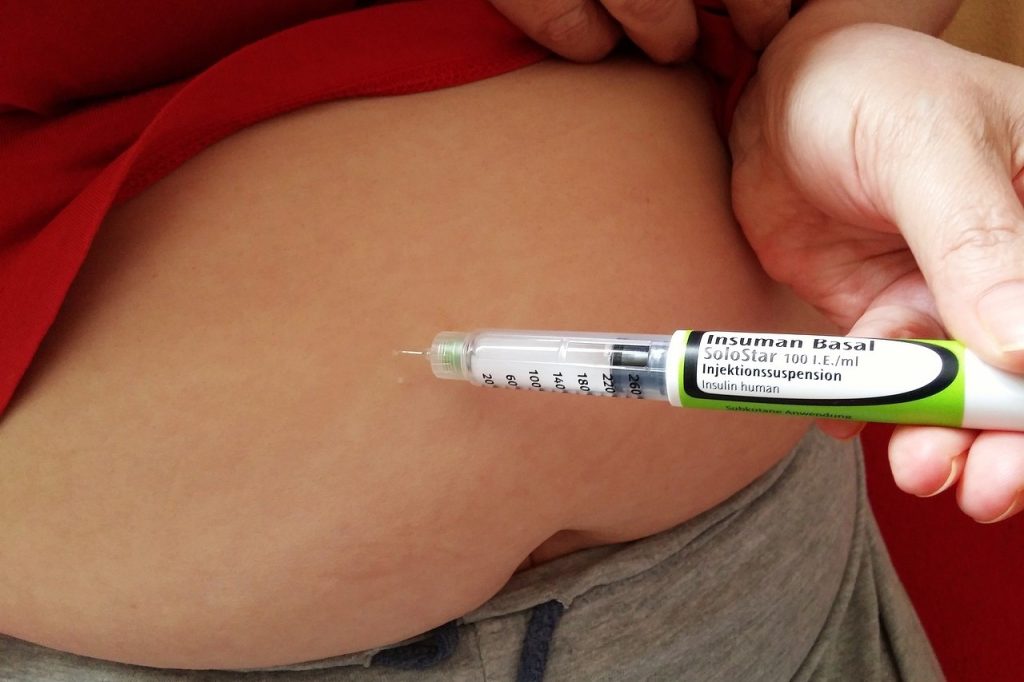
insulin injection
Do you want to know more about insulin? Let’s take a look at these 16 interesting facts about insulin.
- Discovery of Insulin: Insulin was discovered in 1921 by Frederick Banting, Charles Best, and their team at the University of Toronto, revolutionizing the treatment of diabetes.
- Nobel Prize Recognition: Frederick Banting and John Macleod were awarded the Nobel Prize in Physiology or Medicine in 1923 for their role in the discovery of insulin.
- First Successful Treatment: The first successful insulin administration to a human patient occurred in 1922, saving the life of a 14-year-old boy with type 1 diabetes.
- Animal Insulin: Initially, insulin for medical use was derived from animal sources, particularly pigs and cows, before synthetic human insulin was developed.
- Synthetic Insulin: The development of synthetic human insulin in the 1980s transformed diabetes treatment, reducing allergic reactions and enhancing effectiveness.
- Types of Insulin: Insulin comes in various types, including rapid-acting, short-acting, intermediate-acting, and long-acting formulations, each with different onset times and durations.
- Storage Requirements: Insulin must be stored properly, typically refrigerated before opening, and then can be kept at room temperature for a certain period, varying by the specific type.
- Insulin Pumps: Insulin pumps offer an alternative to multiple daily injections, delivering insulin continuously throughout the day, mimicking the function of the pancreas.
- Injection Sites: Common injection sites for insulin include the abdomen, thighs, buttocks, and upper arms, allowing for varied absorption rates.
- Global Access: Despite its importance, access to insulin remains a challenge in many parts of the world due to cost and availability issues.
- Insulin Resistance: Some individuals with type 2 diabetes develop insulin resistance, where cells do not respond effectively to insulin, requiring higher insulin levels for glucose regulation.
- Weight Gain: Insulin therapy can lead to weight gain in some individuals, as it promotes glucose uptake into cells, potentially resulting in increased fat storage.
- Exercise and Insulin: Regular physical activity can improve insulin sensitivity, assisting in better glucose control and reducing the body’s need for insulin.
- Insulin Allergy: While rare, some individuals may develop allergic reactions to insulin, causing skin irritation or more severe responses.
- Critical Hormone: Insulin not only regulates blood sugar levels but also plays a crucial role in the body’s metabolism of carbohydrates, fats, and proteins.
- Continuous Research: Ongoing research aims to develop advanced insulin formulations, such as ultra-rapid-acting insulins or more convenient delivery methods, to further enhance diabetes management.
Insulin, beyond being a hormone, stands as a beacon of hope for millions managing diabetes. Its discovery marked a watershed moment in medical history, saving countless lives and transforming the landscape of diabetes treatment. From its humble origins derived from animals to the synthetic formulations that revolutionized therapy, insulin remains a cornerstone in diabetes management. Despite its pivotal role, challenges persist in ensuring equitable access worldwide. The evolution of insulin therapy continues, propelled by research aimed at improving formulations, delivery methods, and efficacy. As a lifeline for those with diabetes, insulin embodies not just a medication but a symbol of resilience, perseverance, and ongoing scientific progress in the pursuit of healthier lives for all.





